Current Research
Genetics
Neuropsychology
Epidemiology
MRI
Advanced Clinical Neurophysiology
Developing Biomarkers for MND/ALS using Neuro-Electric Signals (EEG)
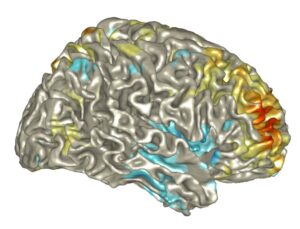
By recording EEG signals during tasks and at rest, researchers within the EXG Research Group and the McMackin Lab at Trinity College Dublin can identify how ALS affects brain function in specific areas and investigate if such abnormalities can be used for new diagnostic tests or to improve the design of clinical trials.
Motor Neurone Disease (MND) causes damage to specific nerves involved in muscle control, called motor neurones. These nerves carry messages from brain regions responsible for movement to the muscle controlling those gestures. MND can also result in changes in other regions, such as those responsible for behaviour and cognition.
The brain is organized to work as networks consisting of interconnected brain cells. Therefore, damage in specific parts of the brain in MND/ALS, disrupts the brain networks more broadly. The degeneration of brain cells (neurons) and the dysfunctional networks are manifested as symptoms affecting movement, breathing, behaviour and cognition.
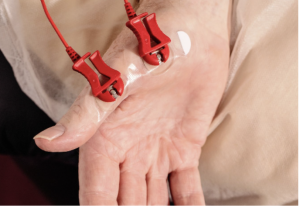
One way to measure the activity of such networks is to use neuroelectric signals such as EEG (electroencephalography, also referred to as brain waves). It is a painless non-invasive procedure using small flat metal discs, called electrodes, attached to a cap worn over the scalp. Those electrodes detect electrical activity in the brain. The next step is to find what brain regions are activated, and how those regions are connected with each other. The measurements of neural signals including EEG and muscle activity (EMG) take place when individuals are at rest (resting-state), when they perform movement tasks or cognitive tasks.
Our aim is to develop novel tools using EEG for the diagnosis of disease categories and measuring the efficacy of new drugs for ALS/MND.
We explore whether we can detect the abnormalities within and between different brain networks in people with ALS/MND using this EEG technology. Changes in the activity and neural communication in specific brain networks can identify different subtypes of ALS/MND that is not yet known to clinicians. Correlating these network disruptions with changes on MRI scanning, psychological and clinical testing and genetic profiles can give us a powerful set of tools that will help us to identify groups of patients with different disease characteristics and help us to understand how genes associated with ALS affect the brain
Abnormalities within and between different brain networks in ALS/MND patients can be used as a marker to make sure that when we develop new drugs, its efficacy is accurately measured, and they are matched to the needs of different subgroups of people with ALS/MND.
Some recent presentations of our work can be viewed below:
Spectral EEG measures identify clusters of ALS patients not discoverable by clinical data.
Cognitive and Auditory Cortical Network Oscillations are Abnormal in ALS.
Longitudinal changes of functional networks disruption in ALS: a resting-state EEG study.
Test-Retest Reliability of EEG markers of Cognition.
Researchers: Dr Narin Suleyman, Ms Eva Woods, , Dr Saroj Bista, Ms Rosie Giglia, Mr Matthew Mitchell, Dr Marjorie Metzger, Mr Prabhav Mehra
Principal Investigators: Professor Orla Hardiman, Dr Bahman Nasseroleslami, Dr Roisin McMackin, Dr Lara McManus
Collaborators: Dr Edmund Lalor (USA), Professor Madeleine Lowery, Professor Richard Carson, Professor Muthuraman Muthuraman (Germany), Dr Stefan Dukic (the Netherlands)
Funders: Health Research Board (HRB), Research Motor Neuron (RMN), Thierry Latran Foundation, The ALS Association, Science Foundation Ireland (SFI), Irish Research Council (IRC), and the Motor Neurone Disease Association in the UK (MNDA)
Volunteering: If you are currently living with MND or are related to two or more people with MND and are interested in taking part in this research or have any questions about this project, please email Aoife Troy (atroy@tcd.ie).
Transcranial Magnetic Stimulation
Developing Measures of MND/ALS using Transcranial Magnetic Stimulation (TMS)
The motor neurons of the brain, which deteriorate in MND, are part of networks of connected brain cells. This means that MND/ALS symptoms may not only result from the loss of motor neurones but also other brain cells which connect with them. One way to measure the activity of the cells in these networks is to use TMS (transcranial magnetic stimulation).
In this test, magnetic pulses are applied to hand movement-controlling cells in the brain. These magnetic pulses cause the cells to activate, sending a message to the hand muscles they control, causing them to very briefly contract, felt as a twitch in the hand. By measuring these twitches with sensors over the skin, we obtain a measure of how well these cells in the brain are working, and how their function is different in those with MND. TMS is non-invasive (no needles) and most individuals report little or no discomfort from these pulses.
These measurements are starting to be used to help in MND diagnosis and testing of new drugs in clinical trials. We are now researching them further in Ireland to improve our understanding of MND and look for measurements which can improve speed of diagnosis and testing of new drugs.
For more information on this research and to see our recent research findings, see www.mcmackinlab.com
Principal Investigators: Dr Roisin McMackin, Professor Orla Hardiman, Professor Richard Carson
Funders: The ALS Association (ALSA), The Motor Neurone Disease Association, Health Research Board (HRB), Research Motor Neuron (RMN) and Irish Research Council (IRC).
Volunteering: If you are interested in taking part in this research or have any questions about this project, please email Roisin McMackin (mcmackr@tcd.ie) or phone 01 896 2718.
Patient and Caregiver Experiences
What is patient and caregiver research?
A diagnosis of MND means different things for different individuals and families. There is no doubting, however, that it transforms the lives of the person with MND and their loved ones.
Over the past number of years, the Research Motor Neurone (RMN) team have carried out studies looking at the experiences of Irish people with MND and their caregivers. In doing this kind of research we aim to
- listen closely to patients and caregivers
- develop care pathways and supports based on what we have heard
- engage in a compassionate way with patients and families that give of their time to take part in research.
Studies of patient and caregiver experience fit under the umbrella of Health Services Research (HSR). Health services research is a multidisciplinary field of enquiry, both basic and applied. Health services research sits at the interface of medicine and human sciences. It asks questions about issues such as how people access healthcare, and how they experience health services. It also looks at how individual, social, and other factors impact on people’s experiences of living with an illness and providing care.
Why is it relevant to MND?
Motor neurone disease is a complex condition; it progresses in different ways for different people. It impacts on each person’s physical health and wellbeing in particular ways. The effect of the condition on a person’s family and social system also varies depending on their circumstances.
Since there is currently no cure for MND, treatments focus on maximising the length and quality of life of those living with the condition. For this reason, it is important to ask questions such as
- what helps people with MND to live as well as possible?
- what supports and treatments make a difference to patients and families as MND progresses?
- what matters to people with MND at different stages in the condition?
- what helps people with MND and their families at end of life?
A related area of research in the RMN team is around the changes in thinking and behaviour that can emerge in MND. This work is covered in the neuropsychology section under the research tab on this site.
What research is happening?
Since MND is a complex condition, our approach to research in MND reflects this. We use a mix of different research methods and designs. We have a variety of researchers with different backgrounds and experience on the team.
Past and current projects are listed below.
- Living and dying with Amyotrophic Lateral Sclerosis: A Population based Analysis of Palliative Needs, Services and Outcomes in non-malignant terminal illness.
- Partners in A Programme for ALS Care in Europe, a project which is following patient and caregiver experiences across Europe to learn about people’s needs and what helps at various stages in the condition. For a recent presentation of some of the work on this project please watch this short video; Individual Quality of Life among Spousal ALS Patient-Caregiver Dyads
- Behavioural Changes in ALS: What Families Need to Know, an educational project for patients and families about changes in thinking and behaviour that can occur in MND.
- Defining and Addressing the Complex Needs of ALS Caregivers, a project that seeks to understand caregivers experience and how changes in thinking and behaviour in MND impact on caregivers. This work was carried out to help us to understand of what kinds of supports are needed by caregivers at different stages in the condition. For a recent presentation of this work please follow the link below; Longitudinal Analysis of Psychological Distress in Motor Neurone Disease Caregivers.
- A Randomised Controlled Study of Psychological intervention in ALS to Address the Significant and Complex Mental Health Needs of Caregivers, a study looking at groups for caregivers and what works best to support their needs at various stages in the condition. Clinical psychologist Ailín O’Dea and researcher Caroline Wheeler have been running groups and are now looking at the findings from these groups. For recent presentations describing some of the work on this project please watch these short videos;
- The IMPACT ALS European Survey Industry Funding On-line survey about living with ALS, approaches to treating ALS, demographics, and caregiver-specific perspectives. Participants: people with ALS (individuals and with assistance as necessary), caregivers (current, former, bereaved); anonymous survey. For a recent presentation of some of the work on this project please watch this short video: People Living with ALS and their Caregivers’ Input into Drug Development in Europe.
- TiM Ireland HRB funding, we are modifying, implementing and evaluating a new patient/caregiver-oriented telemedicine system developed by our collaborators in Sheffield University, to provide immediate virtual support for those with Motor Neuron Disease (MND) and Frontotemporal Dementia (FTD) and related conditions. We will examine the strengths and opportunities for modification of this system, tailoring it to enhance care for Irish patients and their families. For further information on some of the early work on this project please watch the following short presentation: Management of Vulnerable Patients During the COVID-19 Pandemic.
Funders: HRB (Health Research Board), JPND (EU Joint Programme – Neurodegenerative Disease Research), ALSA (ALS Association). Cytokinetics, Biogen, Ionis
Researchers: Dr. Ailín O’Dea, Ms. Caroline Wheeler, Ms. Eilís Conroy, Ms. Sile Carney, Dr. Sinead Maguire, Ms. Polly Kennedy.
Principal Investigators: Professor Orla Hardiman, Dr. Miriam Galvin, Dr. Niall Pender.
Collaborators: Professor Anthony Staines (Health Systems, DCU); Professor Charles Normand (Health Policy and Management, TCD); Dr. Regina McQuillan (Palliative Care, St. Francis Hospice, and Beaumont Hospital); Ms. Bernie Corr (National MND Clinic, Beaumont Hospital); Dr. Katy Tobin (School of Nursing, TCD), Professor Christopher McDermott (Sheffield Institute for Translational Neuroscience); Professor Zachary Simmons (Penn State Hershey Medical Center, Pennsylvania); IMNDA; ALSCarE consortium partners. Dr. Tom Burke; Dr. Jennifer Wilson O’Raghallaigh (Beaumont Hospital); Prof. Leonard van den Berg (UMC Utrecht); Prof. Ammar al Chalabi (Kings College London)
Neuropharmacology and Drug Development
TRICALS
![]()
TRICALS is the largest European research initiative to find a cure for ALS to date. 40 top research centres in 14 countries have joined hands with patient organisations and fundraisers to reach our one goal: find effective treatments for ALS. Research Motor Neurone and the ALS/MND Research Team at Trinity College are delighted to be involved in this exciting initiative which sees the very best experts from top research centres around the globe teaming up with patient organisations, fundraisers and pharma companies in a unique international collaboration to find a cure for ALS.
Amyotrophic Lateral Sclerosis (ALS) is a complex and fatal neurodegenerative disease. The disease is variable between individuals, making every patient unique. It is therefore unlikely that any single scientist, approach or country will be able to find new and effective treatments by themselves.
By uniting our efforts, resources and talents, we will be quicker in realizing our shared ambition: to find effective treatments for ALS. Therefore, patients, top ALS experts and ALS foundations / charities from 14 countries have now joined hands in this unique collaboration on an unprecedented scale.
The success rate of clinical studies testing drugs for ALS has been disappointing. Promising findings from genetically modified animal models have proven difficult to translate to patients due to the complexity and variability of ALS in humans. TRICALS (Treatment Research Initiative to Cure ALS) therefore believes that a radical change in the direction of research is required.
The future must focus on providing effective clinical studies that are designed for subgroups of patients who share specific aspects of the disease. At this moment, however, less than 5% of patients with ALS are eligible to participate in clinical trials. Our goal is to change this, and to give every patient with ALS access to clinical trials, regardless of how long they have had ALS or the type of ALS they have. By doing so, we can accelerate the search for finding effective treatments for ALS patients. Find out more about how we plan to do this by visiting our website The highway towards a cure – TRICALS
Clinical Measurement/Digital Health Technologies
Clinical measurements also allow the health care disciplines to make informed decisions on the optimal care for an individual with Motor Neuron Disease. We also believe that the rate of change is an important parameter to measure. For example if we make two measurements over time and see little change, we know that the rate is slow but if a large change is observed, it may be time to intervene with a treatment that can help.
Our group focuses on three main areas
- Measurement of Lung (breathing and coughing) function
We are conducting studies with European Partners in Belgium, Italy, UK, and The Netherlands to measure lung function over time. We have just completed a two-year study in which we measured lung function over 2 years in 287 participants. We have a large dataset now which will allow us to understand in great detail the impact of Motor Neuron Disease on breathing and the subsequent effects on the individual’s quality of life. Since the onset of the COVID-19 pandemic we also moved rapidly to assessing if it is possible and practical to measure lung function at home. In these evaluations, an individual with Motor Neuron Disease received their own equipment at home to measure their lung function. Then using tele-consultation, a health care professional coaches them through the test and the results can be discussed and a treatment plan decided upon.
Currently we are also investigating new materials that might become easier ways of measuring breathing function. With our engineering partners we have looked at nano-materials and magnetic technologies to see if these could be harnessed to measure lung function in a less obtrusive but equally accurate way to current systems.
- Measurement of Physical Function.
Physical functions include walking, climbing stairs, washing, dressing, driving, writing, talking, swallowing. Breathing is also a physical function (covered above).
The focus of our research in this area is to utilise technology to make sure that the measurements we can obtain about physical function from individuals are exact, can be taken remotely, and are un-obtrusive and easy for the patient and their family. The availability of low-cost sensors and improved technology in homes (computers, electronic tablets, smartphones) means there are huge opportunities to track physical function more accurately. This in turn will improve our understanding of how Motor Neuron Disease affects physical function and inform clinical decisions and treatments. We partner with electronic engineers and computer scientists to investigate how technology can provide us with this information and how we can best process it to improve care.
We also are investigating the use of wearable sensors to track physical activity and how it changes in Motor Neuron Disease. It is exciting to see new wearables that are designed to track fitness coming onto the market at lower prices than the expensive lab-based movement analysis systems that we historically used. Being able to “see” in real life how individuals with Motor Neuron Disease are managing physical activity and deciding what measurements are most useful is one of our research priorities. For example, it may be that step count is important, or perhaps heart rate, or time spent sitting that will best allow us to track the disease.
Our ultimate aim is to be able to provide the right and effective treatment (be it a nursing intervention, a pharmacological (drug) intervention or physiotherapy, occupational therapy, speech and language therapy) at the right time.
- Rehabilitation Interventions
Rehabilitation is essential for those with Motor Neuron Disease. There is often uncertainty at the time of diagnosis about the role of exercise and how much or little individuals should do. As the disease progresses, so do the rehabilitation needs. A focus of our group is to understand the problems associated with rehabilitation, be they problems of access or effectiveness and to develop technology that will help those with MND to participate in exercise programmes safely and with the best exercises. We are planning to build a digital platform which can be a go-to for those with Motor Neuron Disease to get a personalised and effective exercise programme delivered straight to their smartphone to assist them.
Some recent presentations of our clinimetrics work can be viewed by following the links below:
Correlations between measures of ALS respiratory function: Is there an alternative to FVC?
Evaluation of Remote Respiratory Testing implemented in response to the Covid-19 pandemic.
Development of Novel Dexterity Device for Finger Tapping Test
Principal Investigators: The team is led by Dr. Dara Meldrum and Dr. Deirdre Murray.
Collaborators: We work with electronic engineers, computer scientists and are part of a large European network of researchers who meet regularly to share ideas, conduct studies together and plan further research
Funders: We have received funding from the Health Research Board of Ireland (HRB), Research Motor Neurone, Cytokinetics, Enterprise Ireland and the Irish Research Council.
FOLLOW US ON TWITTER
LIKE US ON FACEBOOK
 Research has established that approximately 50% of people with ALS develop some changes in the way they think (cognition) or behave, with approximately 13% of people with ALS developing dementia. The type of dementia associated with ALS is called frontotemporal dementia.
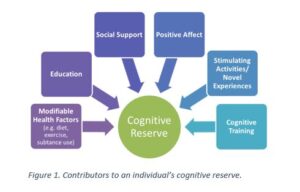
Research has established that approximately 50% of people with ALS develop some changes in the way they think (cognition) or behave, with approximately 13% of people with ALS developing dementia. The type of dementia associated with ALS is called frontotemporal dementia.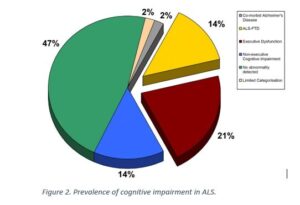 A study, carried out by the Irish MND research group, examined the role of education, occupation and physical activity in protecting against cognitive change in ALS. These three factors are hypothesized to contribute to an individual’s cognitive reserve, which enables an individual to remain cognitively healthy. The study found that individuals with higher cognitive reserve remained cognitively healthy for longer.
A study, carried out by the Irish MND research group, examined the role of education, occupation and physical activity in protecting against cognitive change in ALS. These three factors are hypothesized to contribute to an individual’s cognitive reserve, which enables an individual to remain cognitively healthy. The study found that individuals with higher cognitive reserve remained cognitively healthy for longer.